Could Clinical Trial Reporting Spur Illicit Substance Use?
Might the widespread publicization of oversimplified clinical study findings contribute to increased substance use? The precipitous rise of cannabis legalization, industrialization, and use may prove a powerful case in point. Some studies suggesting the efficacy of cannabis to treat various medical problems were used by cannabis proponents to support the drug’s legalization and commercialization.
In recent years, stories citing small-scale clinical trial data published in traditional and social media channels suggest that cannabis could effectively treat pain and some mental health disorders, and even replace the use of some opioids to help address the opioid epidemic.
More recent information about the effects of legal medical and recreational cannabis calls into question many of the claims made by these earlier studies and highlights the adverse knock-on effects of cannabis legalization, including sharp rises in cannabis use disorder, cannabis induce psychosis, emergency department visits, and traffic accidents.
Importantly, America’s longest-running study on substance attitudes indicates that fewer people than ever feel that cannabis poses health risks, and cannabis use among all age groups, including teens and adolescents, is up.
If it holds true that people’s beliefs about substances and consumption behaviors can be swayed by exposure to clinical trial data (no matter how preliminary and cursory), this may be one reason for recent increases in hallucinogen use.
Data from the Centers for Disease Control and Prevention (CDC) indicate that just this year, clinical trials conducted by highly trusted institutions including Johns Hopkins, Columbia University Irving Medical Center, the University of California at San Francisco, and others, show that hallucinogens like psilocybin and ketamine may reduce the symptoms of treatment-resistant depression, a major public health problem.
The findings of these studies have been circulated by esteemed publications including the New York Times, The Guardian, the BBC, National Public Radio, Stat News, and others. In fact, a Google search for “psilocybin treats depression” returns more than 5.5 million results. While research into the potential mental health benefits of hallucinogens has peaked in recent years, the study of these substances as commercial medications has been underway for decades.
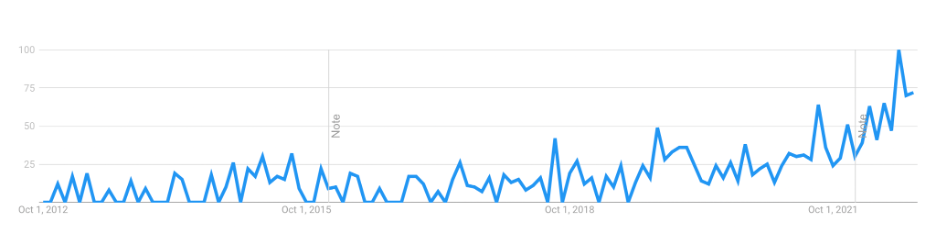
A peer-reviewed study released in August by the Columbia University Mailman School of Public Health and Columbia University Irving Medical Center indicates hallucinogen use grew from 1.7 percent in the U.S. in 2002 to 2.2 percent in 2019.
Just as promising clinical trial data may have spurred increased cannabis use, so too the publication of studies indicating potential health benefits of hallucinogens may reduce perceived health risks and make people feel more comfortable about using these substances.
Part of the problem posed by news reporting about clinical trials is that people may not read beyond the headlines or think critically about the study’s findings. Many of the articles reporting on the trials of psilocybin and ketamine make it clear that trial sample sizes may be small, that additional phases of research are needed to determine if compounds found in these substances can be turned into safe and efficacious medications, and that people should not attempt to achieve the same effects by using these substances on their own.
The Nature article “Psychedelic drugs take on depression — Mind-altering drugs might provide relief for those who don’t respond to conventional therapies — but does the hype outweigh the hope?” questions the significance of some claims made by recent studies suggesting the health benefits of hallucinogens and cites an important fact — that the promising effects of hallucinogens like esketamine show modest differences when compared to placebo. Additionally, many of the clinical trials being conducted are performed under close medical supervision and often include trained psychotherapists who counsel test participants during their study experience.
Despite the fact that most clinical trial reporting contains cautionary language and suggests that further study is needed to substantiate initial findings, it is possible that many readers may simply conclude that the substances are safe or beneficial because they either skim news headlines without reading full articles or choose to make their own interpretations.
As summarized in a 2014 Washington Post article, “Americans read headlines. And not much else.” “So, roughly six in 10 people acknowledge that they have done nothing more than read news headlines in the past week. And, in truth, that number is almost certainly higher than that, since plenty of people won’t want to admit to just being headline-gazers but, in fact, are.” It is possible that even fewer people read in-depth news coverage or follow-up on news stories today — seven years after this article was written.
Before internet-based news and the ubiquitous use of mobile devices, most people got their news through a relatively small number of television and radio channels, newspapers, and periodicals. The relatively high cost of producing and distributing news, and the pressure by advertisers to control the quality of editorial content, meant that most major news outlets spent significant time fact-checking stories, and fewer news stories made it into mass circulation.
Scholarly articles like clinical trial information were most likely to be found in esoteric trade publications read by members of the medical profession rather than in mainstream media. Today, we are exposed to millions of times more sources of information, many sources do not fact-check information, and still, other information channels shape news to suit political or commercial outcomes. Another major change is the algorithmic distribution of information, largely driven by social networks, that attempts to deliver news that evokes an emotional response among consumers (as has been claimed about the inner workings of Facebook).
Confirmation bias is another issue that can impact information consumers and make them more likely to draw their own conclusions when presented with facts. Confirmation bias is the tendency to use information to confirm existing beliefs. If an individual is predisposed to believing that hallucinogens, like psilocybin, are natural substances that are harmless or efficacious, reading headlines that seem to support this point of view can solidify their belief in this supposition despite the fact that this assertion may not be accurate.
Digesting news uncritically and confirmation bias has led people in some quarters to expect a “psychedelic revolution” in the treatment of substance use disorders and other mental health conditions.
“In light of popular media reports of a forthcoming ‘psychedelic revolution’ with commercialization and marketing that may further reduce the public perception of any risk, researchers, clinicians, and policymakers should increase their attention to the rising rates of unsupervised hallucinogen use among the general public,” observed Columbia University study author Deborah Hasin. “Our results highlight such use as a growing public health concern and suggest that the increasing risk of potentially unsupervised hallucinogen use warrants preventive strategies.“
LSD, psilocybin, phencyclidine (PCP), MDMA, and other dangerous hallucinogens are listed in the Diagnostic and Statistical Manual of Mental Disorders (DSM-5) used by psychiatrists in the United States to diagnose substance use disorders. Symptoms of LSD use can include panic attacks, psychosis, seizures, and delusions. Another condition listed in the DSM-5 is cannabis use disorder (CUD), a potentially serious condition frequently requiring treatment.
Treatment providers see the impacts of misleading or misinterpreted substance information
Clinicians at Foundry Treatment Center Steamboat, and colleagues across the country, often witness the collision between incorrect perceptions about psychoactive substances and the negative effects of their problematic use. It is common, for example, for Foundry Steamboat clinicians to find clients experiencing cannabis use disorder surprised to learn that cannabis addiction is possible. The prevailing narrative that cannabis is not habit forming is untrue, and rates of cannabis use disorder and problematic use have increased since the substance became medically and recreationally legal.
Cannabis legalization, commercialization, and use disorder may be a bellwether for the future of hallucinogens and other substances highlighted in clinical studies. The specter of changing public risk perceptions that may increase the likelihood of substance trial and use is worrisome to behavioral healthcare providers.
“When Colorado legalized recreational cannabis, many of us were worried about the results, especially for younger people. Unfortunately, these worries were justified,” says Amber King, Foundry Steamboat Outreach and Special Projects. “We are not only seeing more people finding themselves addicted to high-potency THC products, but we are also seeing other negative impacts in the community. Some of these problems, like increased traffic accidents and children accidentally accessing these products, mirror some of the problems caused by alcohol, which kills more people every year than any other substance.”
“Now we are afraid that the trend toward relaxing concerns about other substances will result in similar problems,” says King. “Widespread headlines that suggest that hallucinogens may help treat mental health conditions could lead some people to attempt to self-medicate with these substances — a choice that without proper clinical supervision and dosages could exacerbate preexisting mental health disorder symptoms instead of alleviating them. Other people may simply believe that using these substances is unlikely to be harmful. Still other people may use this information to push for legalization and commercialization, a move that has had catastrophic effects for many people negatively affected by cannabis legalization.”
The Foundry Treatment Center Steamboat Men’s Program provides comprehensive, Trauma-Integrated Care to men experiencing substance use and co-occurring mental health disorders. The program’s virtual Intensive Outpatient Program treats adults throughout Colorado. For more information call (844) 955-1066.




